Trigeminal neuralgia: case report and literature review
Abstract
Trigeminal neuralgia (TN), also known as tic doloureaux, is a nerve disorder of the face and is considered to be one of the most painful human conditions. A 51-year-old male presented with severe intermittent pain on the left side of his face. Magnetic resonance image scan with contrast revealed a close association of the superior cerebella artery and the trigeminal nerve on the left side of the face. Oral medication is the first line of treatment for TN, because of its non-invasiveness, low cost and high effective rate. Surgical intervention for TN aims to relieve the pressure of the offending artery or vein that is compressing the trigeminal nerve or in other instances; surgery may stop the uncontrolled pain signals. An important criterion for clinical diagnosis is pain that cannot be attributed to another disorder and also the lack of evident neurologic disorder. TN is one of the most debilitating diseases an individual may suffer and an early astute diagnosis of TN will provide patients with relief from suffering, unnecessary dental and medical intervention. Appropriate and early diagnosis of TN is important to formulate an optimal management plan based on the patient’s age and general condition. The aim of this case report is to describe a case of Classical TN, and subsequent successful surgical management with microvascular decompression.
Keywords
Introduction
Trigeminal neuralgia (TN), also known as tic doloureaux[1,2], is considered to be one of the most physically and psychologically painful conditions a human being might suffer[1,2]. Living with TN can have a significant negative impact on a person’s quality of life[3], resulting in problems such as seclusion, weight loss and depression[3,4]. TN is caused by neurovascular conflict[1] which is compression of the trigeminal nerve or an underlying condition that affects this nerve[1,2].
TN causes an abrupt, searing facial pain that shoots within the distribution of one or more branches of the trigeminal nerve[5]. It manifests as a short-lived but intense sudden, severe, brief, stabbing, and recurrent pain[1,5,6].
TN is diagnosed clinically based on the history of symptoms which the patient usually describes as a sudden shooting or stabbing pain, which may be solitary sensations or paroxysms in between pain-free intervals[3,4,6]. TN may be triggered by stimuli that are usually not painful, such as a facial caress, exposure to a gentle breeze, chewing, speaking, or brushing teeth may trigger TN[3,4,6]. In some cases TN may be preceded by facial tingling or numbness prior to the onset of pain[6]. TN in most cases affects a single division and it can later spread to other divisions[7], with specific areas on the face triggering pain when stimulated[4,5]. The attacks of pain occur more frequently and more severely with time[6,7] and may manifest with one or several symptoms such as intense, shooting, stabbing pain that is similar to electric shocks, intermittent twinges of mild pain,spasms of pain, episodes of cluster attacks. TN pain can be focused in a specific area or spread over a widespread area[7,8,9]. TN pain episodes can last from a few seconds to several minutes, usually unilaterally, or less frequently on both sides of the face. The attacks of pain may go into remission and patients maybe symptomless for months or years[5,7]. Women are twice as likely to be affected with this condition as men and in both genders, it is more prevalent after the age of 40 years[1,3], with a prevalence of 4.3 per 100,000[8,10].
TN is classified as classical or symptomatic TN[5,8] and symptomatic TN is caused by disease that leads to neural damage such as multiple sclerosis, herpes zoster, trauma, space-occupying lesion or tumours of the cerebellopalatine angle[2,4]. Classical TN is caused by neurovascular conflict and is divided into type 1 and 2[1,5]. Type 1 is purely paroxysmal and the patient is has no pain in between attacks and type 2 presents with persistent simultaneous, background facial pain between attacks. Type 2 is also known as atypical TN and in this type central sensitization may be responsible for the persistent pain. Neurovascular conflict may not be evident in type 2, and is found to be resistant to several treatment modalities[5,6]. Classical TN is characterized by very severe, sudden, severe excruciating, shock-like pain paroxysms usually on one side of the face at the second and/or third trigeminal branch region[1,2,8]. The typical description is usually volunteered by the patient as a sharp shooting pain similar to having an electric shock in the jaw, teeth or gums[5,6,7,9]. The painusually occurs in erratic attacks which have a duration of a few seconds to about 2 min, and these attacks stop as suddenly as they start[5,6,7,9]. TN usually manifests on one side of the face and the pain is usually felt in all or part of the face. TN does not usually manifest on both sides of the face, however if it does, it is seldom at the same time[5,7,9].
TN attacks of pain can occur on a regular basis for days, weeks or months at a time and in severe cases attacks may occur quite a few times a day[6,7]. TN pain may go in to remission becoming less or sometimes disappearing completely for several months or years at a time, thereafter it emerges more intensely[6,7,9]. The remission periods tend to get progressively shorter and at times develop into a more persistent aching, agonizing and burning sensation, which may or may not be accompanied by bouts of sharp attacks[4,6,8].
The aims of this case presentation is to describe a case of classical TN, and subsequent successful management with microvascular decompression (MVD) as appropriate and early diagnosis of this debilitating condition is imperative in formulating an optimal management plan.
Case report
A 51-year-old male presented with a main complaint of severe, sharp, piercing intermittent electrical-like shock pain on the left side of his face. The pain was triggered by talking, washing his face, eating and brushing of his teeth and the patient VAS score was four. No pathology was detected during the intra and extra oral examination except clicking of the temporomandibular joint associated with opening and closing jaw movement.
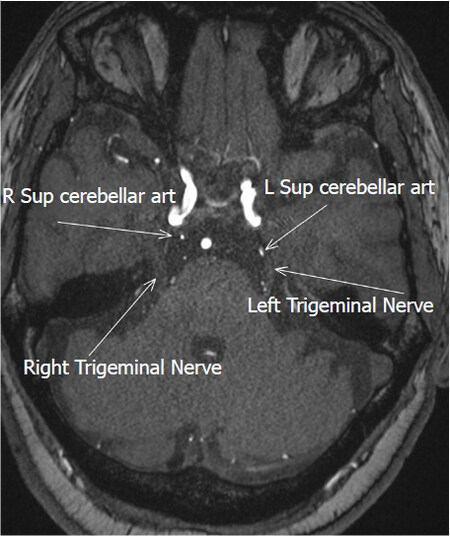
Patient had a history of temporomandibular joint pain previously (about 20 years ago) which was treated and had resolved. Radiological investigation revealed no abnormalities and the patient had no history of diabetes mellitus, high blood pressure, chronic heart diseases, hepatitis, or any other pertinent chronic diseases. A provisional diagnosis of TN was made which was confirmed by an magnetic resonance image (MRI) scan with contrast, which revealed a close association of the superior cerebellar artery and the trigeminal nerve on the left side [Figure 1].
Figure 1. MRI scan with contrast which revealed close association of the superior cerebellar artery and the trigeminal nerve on the left side.The label of the left superior cerebellar artery points to the exact point of where the artery is in contact with the left trigeminal nerve. When compared to the right there is significant distance between the right trigeminal nerve and the right superior cerebellar artery. MRI: magnetic resonance imaging
The treatment options of medication and surgery was discussed with the patient and blood samples were taken from the patient for a full blood count, carbamazepine level analysis and to test liver function, which were found to be normal. Carbamazepine (Tegretol® 200 mg twice daily) was prescribed and the patient volunteered that he was pain free at the recall appointment a month later, at which time the patient was found to be coping and symptom free.
The same patient presented a year later with neuralgic pain which started 3 weeks prior. The patient reported that the episodes of pain had increased in severity and frequency, with a longer duration lasting several minutes and increased in intensity. The patient further reported side effects from the medications which were impacting negatively on his physical, social, and psychological function. Considering the patient’s current reduced quality of life, pain intensity and the ineffectiveness of the medication, the expected chance of a successful outcome of the surgical interventions was weighed against the potential surgical complications for the intervention. Neurosurgical treatment was recommended to the patient and information about the efficacy and potential complications for each type of surgical intervention was given by the treating neurosurgeon in the presence of a close relative, verbally and in writing. A full blood analysis, carbamazepine levels and liver function tests were done and found to be within normal ranges, thereafter baclofen (Lioresal, 5 mg three times daily) was prescribed for the patient.
The patient then presented two weeks later with breakthrough pain stating that the condition had become unresponsive to the medication and the pain had become unbearable. He further complained of being woken up from several times from sleep (± 5 times daily) by severe pain possibly triggered by the stimuli of the pillow rubbing his face when changing his sleeping position. The patient then requested the option of MVD procedure and three weeks later was successfully treated with MVD. The patient’s symptoms resolved postoperatively without complications and there has been no reports of neuralgic attacks at the 1st and 2nd years follow up visits.
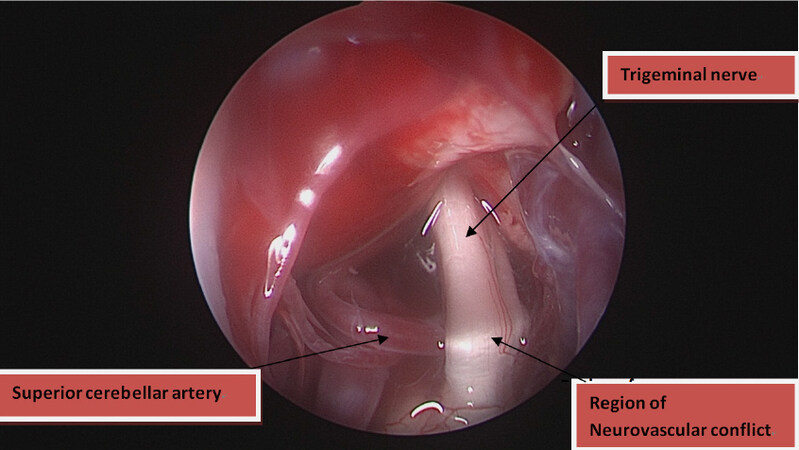
MVD was considered to be the best surgical treatment because a neurovascular conflict was identifiable on the MRI and the patient was screened and found to be stable enough to undergo open neurosurgery. In MVD, the target area lies at the nerve-pons junction. A suboccipital craniotomy was performed to access the posterior fossa. The cerebrospinal fluid was aspirated and then the superolateral margin of the cerebellum was gently retracted to gently expose the nerve. The nerve was found to be compressed by a loop of the superior cerebellar artery at the root entry zone [Figure 2].
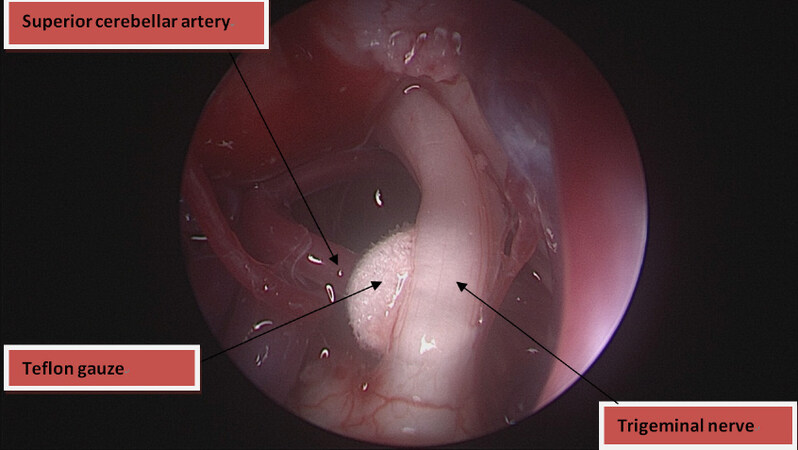
The arachnoid was then dissected and the vessel including the entire root, from meckel’s cave to the trigeminal root entry zone, was freed from all arachnoid adhesions. A piece of shredded Teflon gauze was placed between the vessel and the nerve to completely separate the two [Figure 3].
Figure 3. Microscopic image showing the Teflon gauze in place between superior cerebellar artery and the trigeminal nerve
The patient’s symptoms resolved postoperatively without complications and there has been no report of neuralgic attacks at the last follow up visit.
Discussion
According to the international guidelines[10] on TN treatment carbamazepine and oxycarbamazepine is recommended as first line treatment based on clinical studies[1,11,12]. Oral medication, due to its non-invasiveness, low cost and high effective rate is the first line of treatment which involves prescribing anticonvulsant[12,13]. Medication in the form of analgesics (paracetamol and aspirin) and anti-inflammatory tablets (ibuprofen) are ineffective for TN pain[13,14]. Anticonvulsants commonly used for TN are: carbamazepine (Tegretol, Carbatrol, Epitol)[13,14,15], oxycarbazepine (Trileptal )[16], baclofen (Lioresal)[17], gabapentin (Neurontin), valproic acid (Depakene, Depakote), phenytoin (Dilantin), topiramate (Topamax) and lamotrigine (Lamictal)[7,10] which have been found to be effective as various combination treatments or stand alone treatments for TN[11,14,15]. Common adverse effects of anticonvulsants include: nausea, dizziness, confusion, drowsiness, vision problems, suicidal thoughts and allergies[15,16,17].
The international guidelines[10] further state that surgery would be a reasonable next step in the case where sodium-channel blockers (carbamazepine or oxcarbazepine) are ineffective[10,12] thus invasive treatments can be considered and implemented depending on the suitability of the patient for the procedure[10,12,18]. Surgery intervention for TN aims to relieve the pressure of the offending artery or vein from compressing the trigeminal nerve[15,16,17] or in other instances surgery may stop the uncontrolled pain signals by damaging the trigeminal nerve[12,19,20] which may also lead to temporary or permanent facial numbness[8].
There are a number of surgical options available to effectively treat TN which include percutaneous glycerol rhizotomy (PGR), percutaneous balloon compression (PBC), percutaneous stereotactic radiofrequency thermal rhizotomy (PSRTR), gamma-knife radiosurgery (GKR), partial sensory rhizotomy (PSR) and MVD[8,21-23].
Surgery can provide good relief, but relapse may occur within months or years later[8,20]. According to the literature most cases, up to 95% of cases of TN is caused by an artery or vein compressing the trigeminal nerve[8,20,21]. The area of pain in classical TN will depend on which of the three branches of the trigeminal nerve is affected, though more than one branch at a time can be affected[8,22,2]. The ophthalmic branch has an effect on the forehead, nose, and eyes; the maxillary branch has an effect on the lower eyelid, eyes, side of nose, cheek, upper gum, upper lip, and upper teeth[8,22,23]. The mandibular branch has an effect on the lower jaw, teeth, gum, and lip[8,22,23].
Oral medication is usually the first line of treatment of Classical TN due to its high effective rate, none-invasiveness and low cost[8,12]. The international guidelines[10] on TN treatment recommends carbamazepine[13] and oxcarbazepine[16], baclofen[17], pregabalin, lamotrigine and gabapentin[13,14] which have been found to be effective as various combination treatments or stand alone treatments for TN[10,24]. There are a number of surgical options available to effectively treat TN which include PGR, PBC, PSRTR, GKR, PSR and MVD[8,22,23].
PGR is a procedure also known as a glycerol injection, is performed under mild sedation and local anaesthesia. A little quantity of sterile glycerol is injected damaging the trigeminal nerve, and thus blocking the pain signals[8,23]. An opening at the base of the skull is accessed by inserted a needle through the face which is then guided by imaging techniques to the joining point of the three branches of the trigeminal nerve[8,23]. This procedure uses similar trajectories as in radiofrequency lesioning and balloon compression where the needle is inserted into the trigeminal cistern through the foramen ovale[8,23]. The majority of people experience immediate and significant pain relief with PGR, though pain may recur later. A common side effect of PGR is facial tingling or numbness[8,23].
PBC of the trigeminal nerve is a procedure where a hollow needle is used to place a balloon next to the nerve which is then inflated. In almost all the patients there is only a mild sensory loss with immediate pain relief [8,23].
PSRTR destroys specifically selected nerve fibres linked to pain by means of electrical currents by means of an electrode which is attached to the nerve root under sedation thereafter the patient awakened from sedation to determine whether they can feel the electrical pulses. The patient is then sedated again and the nerve is destroyed by heating the electrodes[8,19]. A common side effect of PSRTR will experience some facial numbness afterward[19].
GKR is a technique that aims a high dose of radiation at the root of the trigeminal nerve, gradually resulting in damage to the nerve. Pain relief will gradually take place over several weeks however the initial pain relief may take a few weeks to effect. Most patients are successfully treated with GKR though some patients may experience a relapse[21,22].
PSR entails making a perforation in the skull and the nerve is severed or at times rubbed, which results in the patient having permanent facial numbness.
MVD is a surgical procedure that entails placing Teflon gauze between the nerve and any offending arteries or veins, effectively separating them away from the nerve[25,26]. MVD is a safe and effective procedure due to developments in surgical techniques,use of operation microscope and advances in neuro anaesthesia[26,27,28]. In MVD, the posterior fossa is approached through a suboccipital craniotomy to access the target area at the nerve-pons junction[26,27,28]. The cerebrospinal fluid is aspirated, then operator advances toward the nerve by gently retracting the superolateral margin of the cerebellum[26,27,28]. The offending vessel is usually the superior cerebellar artery and less frequently, the anterior inferior cerebellar artery or the superior petrosal veins which compress the nerve at the root entry zone[20,22,26]. The arachnoid is then dissected and the vessel freed, then the surgeon inserts a piece of shredded Teflon gauze between the offending vessel and the nerve to separate them[26,27,28].
MVD can be performed on patients of any age provided the patient is screened and found to be stable enough to undergo general anaesthesia. Retrospective studies showed that pain relief and complications were not age dependant[8,26,29,30] as in this case, most patients (87%-98%) experienced immediate pain relief[20,29,30] the initial success rate of 85 to 95% with a recurrence rate of 20% and 30%, at 6 and 10 years[23,29,30]. Though results from definite arterial compression are better, a recurrence rate of 31% has been reported usually occurring within the first 12 months of the operation in patients with TN caused by venous compression. In cases of recurrence, re-exploration and neuroablative procedures have been recommended for remedial action[26,29,30]. MVD is not associated with any sensory loss[29], however reported complications are eighth nerve injury in 0.8%, cerebellar injury was reported in 0.45%, and cerebrospinal fluid leak in 1.85%[8,29,30]. It is imperative that patients should be monitored postoperatively to screen for complications such as corneal abrasions and anaesthesia dolorosa[8,29,30].
Pharmacotherapy with anti convulsants such as oxycarbamazepine or phenytoin is worth trying in the first instance as the initial therapyand is often sufficient and effective for 75% of patients[3,5,21]. Invasive surgery procedures is thus a consideration if pharmacologic treatment fails and the patient is a good candidate for surgery[3,5,21]. TN is a chronic condition that requires long term monitoring and when pharmacotherapy therapy is instituted,a full blood analysis, carbamazepine levels and liver function tests are required[12,13] prior to commencement for a baseline. On commencement of the treatment full liver function and carbamazepine levels should be monitored closely, that is after the first two weeks and then every three months[13,14,15] and whenever the dose is adjusted or adverse effects appear, and annually thereafter[13].
Oxcarbazepine has fewer side effects, but it can cause hyponatremia, thus necessitating monitoring with serial serum sodium measurements in the first few weeks after initiating therapy[14,15]. The option of increasing the dosage of the medication, or the addition of a second anticonvulsant medication, should be considered in patients who experience breakthrough pain[17]. In cases where the patients are young (< 60 years at onset) or patient becomes non responsive to medication, early neurosurgical treatment should be considered, regardless of a negative brain MRI[3,4,21]. Holistic, individualised care is imperative when considering neurosurgery[4,5,21] as surgery that can provide complete relief for many years, if not permanently, excluding the need for anticonvulsant medications and excludes the impact of medication side effects[26,27].
Trigeminal nerve compression will not always present with pain symptoms and it has been suggested that in the symptomatic cases, the pressure on the nerve causes demyelination which is the wearing away of the protective outer layer referred to as the myelin sheath[7,20,21]. This demyelination causes uncontrollable pain signals to manifest along the nerve, though this fails to adequately explain why asymptomatic remission can occur and why there is immediate pain relief post operatively after removal of a blood vessel away from the nerve[20,21,30]. Management of TN must be tailored individually, early diagnosis and prompt referral for specialised care is thus imperative[8,12,22]. A lack of efficacy or intolerable side effects to oral medication justifies the recommendation of neurosurgical treatment to the patient[12,22]. The patient must be educated of the relative efficacy of various modalities of treatments, including complications and recurrence rates[12,23,24]. In this case the expected benefits of surgery outweighed the risks, given the patient’s quality of life, pain intensity and side effects with respect to physical, social and psychological functions. The results of the MRI scan which indicated neurovascular contact and the efficacy and potential complications of neurosurgery were explained and discussed with the patient. Given there was no contra indication to open neurosurgery, MVD was the choice of surgical treatment in anticipation of a permanent cure.
According to The International Headache Society clinical criteria for TN diagnosis[10], a diagnosis of TN can be made when at least three attacks of unilateral facial pain occur fulfilling these criteria:
attacks occurring in one or more divisions of the trigeminal nerve, with no spread of pain beyond the trigeminal distribution and;
pain with at least three of the following four characteristics:
A decisive factor in the clinical diagnosis is pain that cannot be ascribed to another condition and also the lack of evident neurologic disorder[3,11,21]. An MRI of the brain plays an significant role in the diagnosis and presurgical evaluation of TN, especially in assisting in identification of the cause of TN, such as the neurovascular conflict or secondary causes of TN[11,21]. The list of differential diagnoses includes a number of other causes of orofacial pain and headaches such as tumours (meningiomas, acousticneuromas), headache disorders (cluster headache, trigeminal autonomic cephalalgia), dental pain (fractured tooth, dental infection), tempo-mandibular joint disorders, eyes, nose (sinusitis) and other neuralgias (glossopharyngeal, occipital and post-herpetic), and atypical facial pain[3,11,21]. The diagnosis of TN is almost entirely based on the patient’s history and as in most cases of facial pain, no specific laboratory tests are needed, and other possible diagnosis are eliminated after taking a good history and clinical examination[4,5,21].
Classical TN is in most instances diagnosed on the basis of typical history and clinical features however, vascular compression is usually identified with high-resolution MRI[11,21] which is also useful to detect any secondary causes like multiple sclerosis or tumours. Preoperative magnetic resonance tomographic angiography is recommended as useful in patient selection and prognostic for MVD[4,8,21]. Quantitative sensory testing, electrophysiological and evoked potentials studies can also assist in identifying symptomatic TN, though it is not used routinely[3,4,21]. Classical TN has to be differentiated from other possible reasons why a patient presents with trigeminal nerve can become compressed or damaged[4,8,21]. Neuralgia pain is not always indicative of TN as other causes may give rise to neuralgia pain. A thorough examination and radiological investigation is vital in the identification of the cause of pain and is almost entirely based on the patient’s history and generally, no specific laboratory tests are needed[4,11,29]. A good history and clinical examination are paramount to the diagnosis of TN which has to be differentiated from other possible reasons why a patient presents with orofacial pain and headaches[11,12,21]. When reaching a diagnosis and treatment plan for TN, it is important to consider other possible causes of damage or compression of the trigeminal nerve, such as a tumour, a cyst, arteriovenous malformation, physical damage to the nerve due to trauma, a dental or surgical treatment, or infection[11,12,21]. Another consideration is multiple sclerosis a long-term condition that affects the nervous system due to demyelization of the nerve[4,29,30], however in most cases of classical TN the pain is predominately associated with compression of the trigeminal nerve by the superior cerebella artery[21,30].
This case highlights a case of persistent breakthrough symptoms of TN which required a good diagnosis, patient education and follow up strategy. The remarkably positive outcome attained, despite the severity of the symptoms and non-responsiveness to medication highlights the importance of individualizing the management plan according to the patient’s circumstances and the need for a holistic team approach to patient treatment.
TN is one of the most debilitating diseases an individual may suffer and an astute diagnosis of TN will save some patients from suffering, unnecessary dental and medical treatments. MVD being a conservative method can be considered the gold standard and in the field of surgery MVD can be considered a safe and effective treatment for patients with typical TN that are not responsive to pharmacological therapy and are good candidates for surgery. After a successful MVD, many patients awaken without pain and remain pain-free while in other cases the pain resolves gradually during the week or two after operation. This case underlines the value of adequately educating caregivers about facial pain and appropriate referrals, which is in the best interest of the patient.
In conclusion, the originality of the present case rests on the fact that despite the severity of the symptoms and non-responsiveness to medication, a remarkably positive outcome was attained. This presents a strong case for MVD intervention particularly where a high-resolution MRI clearly demonstrates vascular compression. MVD should be considered as the first surgical choice when the patient’s conditions are satisfactory though it is essential that high-quality evidence that compares different modalities of treatments is available to provide a reliable and balanced selection of high-quality evidence that can enable patients, physicians, and health policy makers to select the most effective and efficient treatment.
Declarations
AcknowledgementsWe gratefully acknowledge the patient for giving the necessary permission to report this case. We also gratefully acknowledge radiologist, Dr. Werner Harmse; IT manager, Mr. Charles De Wit and IT specialist, Mr. Ashton Takoor Persadh from Kauffman & Partners Inc. for their valuable contribution in interpretation and report of the MRI findings.
Authors’ contributionsInvolved in conception, design, research and manuscript writing of the study: Turton M
Contributed in performing the operation, provided administrative and technical support: Malan-Roux P
Availability of data and materialsNot applicable.
Financial support and sponsorshipNone.
Conflict of interestAll authors declared that there are no conflicts of interest.
Ethics approval and consent to participateInformed consent has been obtained and this report was processed according to the principles expressed in the Declaration of Helsinki.
Consent for publicationNot applicable.
Copyright© The Author(s) 2019.
REFERENCES
1. Maarbjerg S, Di Stefano G, Bendtsen L, Cruccu G. Trigeminal neuralgia - diagnosis and treatment. Cephalalgia 2017;37:648-57.
3. Montano N, Conforti G, Di Bonaventura R, Meglio M, Fernandez E, et al. Advances in diagnosis and treatment of trigeminal neuralgia. JAAPA-J Am Acad Phys 2015;11:289-99.
5. Nurmikko TJ, Eldridge PR. Trigeminal neuralgia-pathophysiology, diagnosis and current treatment. Br J Anaesth 2001;87:117-32.
6. Rasmussen P. Facial pain. II. A prospective survey of 1052 patients with a view of: character of the attacks, onset, course, and character of pain. Acta Neurochir (Wien) 1990;107:121-8.
7. Mueller D, Obermann M, Yoon M-S, Poitz F, Hansen N, et al. Prevalence of trigeminal neuralgia and persistent idiopathic facial pain: a population-based study. Cephalalgia 2011;31:1542-8.
8. Yadav YR, Nishtha Y, Sonjjay P, Vijay P, Shailendra R, et al. Trigeminal neuralgia. Asian J Neurosurg 2017;12:585-97.
9. Sekula RF, Frederickson AM, Jannetta PJ, Bhatia S, Quigley MR, et al. Microvascular decompression in patients with isolated maxillary division trigeminal neuralgia, with particular attention to venous pathology. Neurosurg Focus 2009;27:E10.
10. Cruccu G, Gronseth G, Alksne J, Argoff C, Brainin M, et al; American Academy of Neurology Society; European Federation of Neurological Society. AAN-EFNS guidelines on trigeminal neuralgia management. Eur J Neurol 2008;15:1013-28.
12. Gronseth G, Cruccu G, Alksne J, Argoff C, Brainin M, et al. Practice parameter: the diagnostic evaluation and treatment of trigeminal neuralgia (an evidence-based review): report of the Quality Standards Subcommittee of the American Academy of Neurology and the European Federation of Neurological Societies. Neurology 2008;71:1183-1190.
14. Taylor JC, Brauer S, Espir ML. Long-term treatment of trigeminal neuralgia with carbamazepine. Postgrad Med J 1981;57:16-8.
16. Zakrzewska JM, Patsalos PN. Oxcarbazepine: a new drug in the management of intractable trigeminal neuralgia. J Neurol Neurosurg Psychiatry 1989;52:472-6.
17. Fromm GH, Terrence CF, Chatta AS. Baclofen in the treatment of trigeminal neuralgia: double-blind study and long-term follow up. Ann Neurol 1984;15:240-4.
18. Spatz AL, Zakrzewska JM, Kay EJ. Decision analysis of medical and surgical treatments for trigeminal neuralgia: how patient evaluations of benefits and risks affect the utility of treatment decisions. Pain 2007;131:302-10.
19. van Loveren H, Tew JM Jr, Keller JT, Nurre MA. A 10-year experience in the treatment of trigeminal neuralgia. Comparison of percutaneous stereotaxic rhizotomy and posterior fossa exploration. J Neurosurg 1982;57:757-64.
20. Marc Sindou. Trigeminal neuralgia: a plea for microvascular decompression as the first surgical option. Anatomy should prevail ActaNeurochirurgica 2010;152:361-364.
21. Maarbjerg S, Gozalov A, Olesen J, Bendtsen L. Trigeminal neuralgia - a prospective systematic study of clinical characteristics in 158 patients. Headache 2014;54:1574-82.
22. Zakrzewska JM, Akram H. Neurosurgical interventions for the treatment of classical trigeminal neuralgia. Cochrane Database Syst Rev 2011;9:CD007312.
23. Tatli M, Satici O, Kanpolat Y, Sindou M. Various surgical modalities for trigeminal neuralgia: literature study of respective long-term outcomes. Acta Neurochir (Wien) 2008;150:243-55.
24. Cruccu G, Truini A. Refractory trigeminal neuralgia.Non-surgical treatment options. CNS Drugs 2013;27:91-6.
25. Hannan C, Shoakazemi A, Quigley G. Microvascular Decompression for Trigeminal Neuralgia: A regional unit's experience. Ulster Med J 2018;87:30-3.
26. Lei Xia, Jun Zhong, Jin Zhu, Yong-Nan Wang, Ning-Ning Dou, et al. Effectiveness and Safety of Microvascular Decompression Surgery for Treatment of Trigeminal Neuralgia: A Systematic Review. J Craniofac Surg 2014;25:1413-7.
27. Sindou M, Leston JM, Decullier E, Chapuis F. Microvascular decompression for primary trigeminal neuralgia: long-term effectiveness and prognostic factors in a series of 362 consecutive patients with clearcut neurovascular conflicts who underwent pure decompression. J Neurosurg 2007;107:1144-53.
28. Sindou M, Leston J, Howeidy T, Decullier E, Chapuis F. Microvascular decompression for primary trigeminal neuralgia (typical or atypical). Long-term effectiveness on pain; prospective study with survival analysis in a consecutive series of 362 patients. Acta Neurochir 2006;148:1235-45.
29. Sekula RF Jr, Frederickson AM, Jannetta PJ, Quigley MR, Aziz KM, et al. Microvascular decompression for elderly patients with trigeminal neuralgia: a prospective study and systematic review with meta-analysis. J Neurosurg 2011;114:172-9.
Cite This Article
Export citation file: BibTeX | RIS
OAE Style
Turton M, Malan-Roux P. Trigeminal neuralgia: case report and literature review. Stomatological Dis Sci 2019;3:7. http://dx.doi.org/10.20517/2573-0002.2019.08
AMA Style
Turton M, Malan-Roux P. Trigeminal neuralgia: case report and literature review. Stomatological Disease and Science. 2019; 3(-1): 7. http://dx.doi.org/10.20517/2573-0002.2019.08
Chicago/Turabian Style
Turton, Mervyn, Pieter Malan-Roux. 2019. "Trigeminal neuralgia: case report and literature review" Stomatological Disease and Science. 3, no.-1: 7. http://dx.doi.org/10.20517/2573-0002.2019.08
ACS Style
Turton, M.; Malan-Roux P. Trigeminal neuralgia: case report and literature review. Stomatological. Dis. Sci. 2019, 3, 7. http://dx.doi.org/10.20517/2573-0002.2019.08
About This Article
Copyright
Data & Comments
Data
 Cite This Article 81 clicks
Cite This Article 81 clicks












Comments
Comments must be written in English. Spam, offensive content, impersonation, and private information will not be permitted. If any comment is reported and identified as inappropriate content by OAE staff, the comment will be removed without notice. If you have any queries or need any help, please contact us at support@oaepublish.com.